NOW AVAILABLE: APCD-CDL™ Version 4.0.1
- APCD-CDL Version 4.0.1 (clean)
- APCD-CDL v4 Changelog
- APCD-CDL Version 4.0.1. (redline) and APCD-CDL Version 4 (redline)
Background
The purpose of the All-Payer Claims Database Common Data Layout (APCD-CDL™) is to harmonize the claims collection effort across states and reduce the burden of data submission. The overall goals of this effort are to improve efficiency, reduce administrative costs and improve accuracy in claims data collection.
The APCD-CDL consists of technical specifications and multiple file layouts composed of data elements, data types, maximum field lengths, descriptions, valid values, and references to industry standards. APCD-CDL files collect adjudicated medical, pharmacy, and dental claims data for all eligible members, with data about members and providers.
- Member Eligibility: demographic data for members eligible for medical, pharmacy, and dental benefits, including references to ASC X12 270/271 implementation guides.
- Medical Claims: service-level remittance with clinical diagnosis codes, medical procedure codes, and charges and payments data, including references to the ASC X12 Post Adjudicated Claims Data Reporting Guides (Institutional and Professional).
- Pharmacy Claims: service-level remittance with drug-dispensing, pharmacy and prescribing physician, and charges and payments data, including references to the NCPDP Uniform Healthcare Payer Data Standard Implementation Guide.
- Dental Claims: service-level remittance with clinical diagnosis codes, dental procedure codes, teeth treated, and charges and payments data, including references to the ASC X12 Post Adjudicated Claims Data Reporting Guide (Dental).
- Providers: provider identifiers, such as the National Provider Identifiers (NPI), with provider name, practice location(s), and specialty data for all providers on all other files.
- Header and Trailer Records: support successful data exchange.
Maintenance Process
We communicate the maintenance process through the website. The process is evaluated and updated during the second quarter of the off-year.
An advisory committee of volunteer state agencies, payers, and vendors established guidelines for maintaining the APCD-CDL:
- APCD-CDL is maintained on a biennial cycle
- Anyone using the APCD-CDL can make a Data Maintenance Request (DMR)
- Corrections to APCD-CDL are made as needed
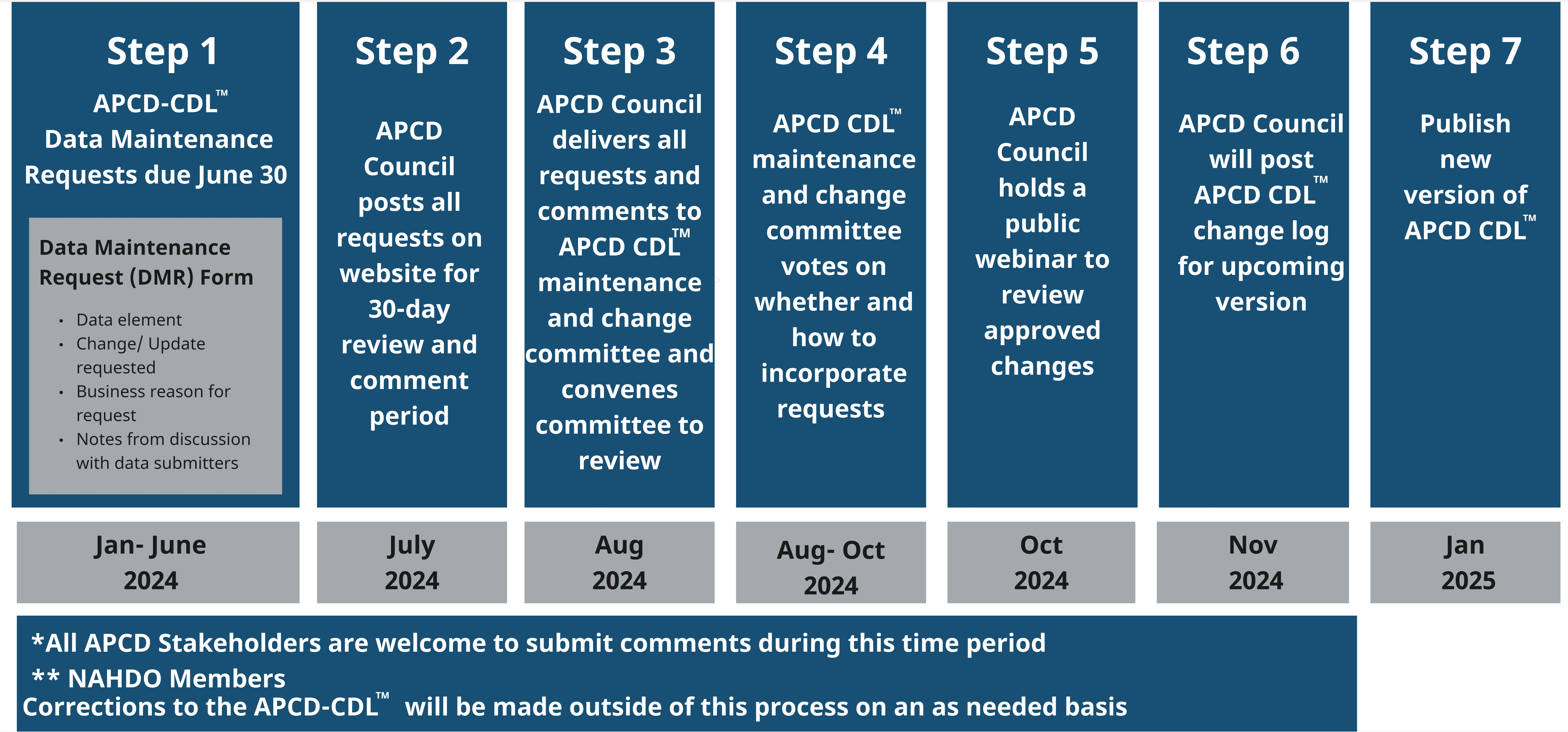
Every other July, APCD Council will post all requests online for a 30-day comment period. ACPD Council will organize and convene the APCD-CDL Maintenance Committee to review requests and comments and vote on changes to the APCD-CDL. APCD Council hosts a review of recommended changes with stakeholders. Final changes are incorporated into a new version of the APCD-CDL published at the beginning of the following year.
APCD-CDL Maintenance Process